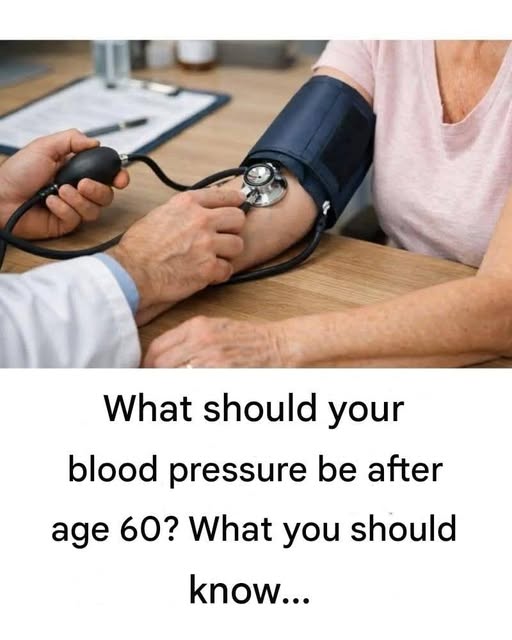
Blood pressure recommendations for people over 60 are based on the same medical principles as for younger adults, but doctors sometimes adjust targets depending on overall health, frailty, and medication tolerance.
Normal Blood Pressure (All Adults)
Modern guidelines from major health organizations say that a healthy blood pressure for adults of any age is below 120/80 mmHg. This is considered the ideal range because it is linked with the lowest risk of heart disease and stroke. However, in real life, many older adults naturally have slightly higher readings.

Typical Blood Pressure in People Over 60
As people age, arteries become stiffer, which often causes the top number (systolic pressure) to rise while the bottom number stays similar or even lowers.
A common pattern in older adults is:
Slightly higher systolic (120–140+)
Normal or lower diastolic (60–80)
This is called age-related systolic hypertension, and it is very common after 60.
When Blood Pressure Is Considered High After 60
The medical threshold does NOT change just because of age:
Normal: below 120/80
Elevated: 120–129 / below 80
High (Stage 1): 130–139 / 80–89
High (Stage 2): 140+/90+
So even at age 60+, a reading like 140/90 is still considered high, not “normal aging.”
What Doctors Sometimes Accept in Older Adults
Even though targets are the same, doctors may adjust treatment goals for some seniors:
Some healthy seniors aim for below 130/80
Frail or very elderly patients may have slightly higher targets (to avoid dizziness or falls from medication)
The key idea is balance: lowering risk of stroke while avoiding side effects like fainting or weakness.
When Blood Pressure Becomes Dangerous
No matter your age, these levels are concerning:
180/120 or higher: medical emergency (hypertensive crisis)
Consistently 140/90+: long-term risk for heart and brain damage
Important Insight
A common misconception is: “High blood pressure is normal when you get older.” That is not true.
What actually happens is:
It becomes more common, not harmless
Risk of stroke, heart attack, and kidney disease increases with age if untreated
Factors That Affect Blood Pressure After 60
Blood pressure in older adults is influenced by more than age alone. Several lifestyle and health factors play a major role in whether readings stay stable or become elevated over time.
Diet and Salt Intake
One of the biggest contributors is sodium (salt). High salt intake can cause the body to retain fluid, which increases pressure in the blood vessels. Processed foods, canned meals, and fast food are common hidden sources of sodium. A diet rich in fruits, vegetables, whole grains, and lean proteins—often referred to as the DASH diet—is frequently recommended to help manage blood pressure naturally.
Physical Activity
Regular movement helps keep the heart and blood vessels healthy. Even moderate activities like walking, swimming, or light cycling can improve circulation and reduce systolic pressure over time. For people over 60, consistency matters more than intensity. Short daily walks are often more beneficial than occasional intense exercise.
Weight and Metabolism
Carrying extra body weight increases strain on the heart. As metabolism slows with age, weight gain becomes more common, which can contribute to higher blood pressure. Even modest weight loss can lead to noticeable improvements in readings.
Conclusion
After 60, the healthiest goal is still:
– around or below 120/80 mmHg (if tolerated)
But in real medical practice, targets may be individualized depending on health condition, medications, and risk of falls.