Dyshidrotic eczema — also known as pompholyx or dyshidrosis — is a skin condition that mainly affects the hands and feet. It causes small, fluid-filled blisters (sometimes described as looking like “tapioca bumps”) to form on the palms, the sides of fingers, and the soles or sides of toes. These blisters tend to come and go. An episode may last a couple of weeks and then fade, only to return later. Despite how it looks, dyshidrotic eczema is not contagious — you cannot catch it from someone else.
Symptoms and What It Feels Like
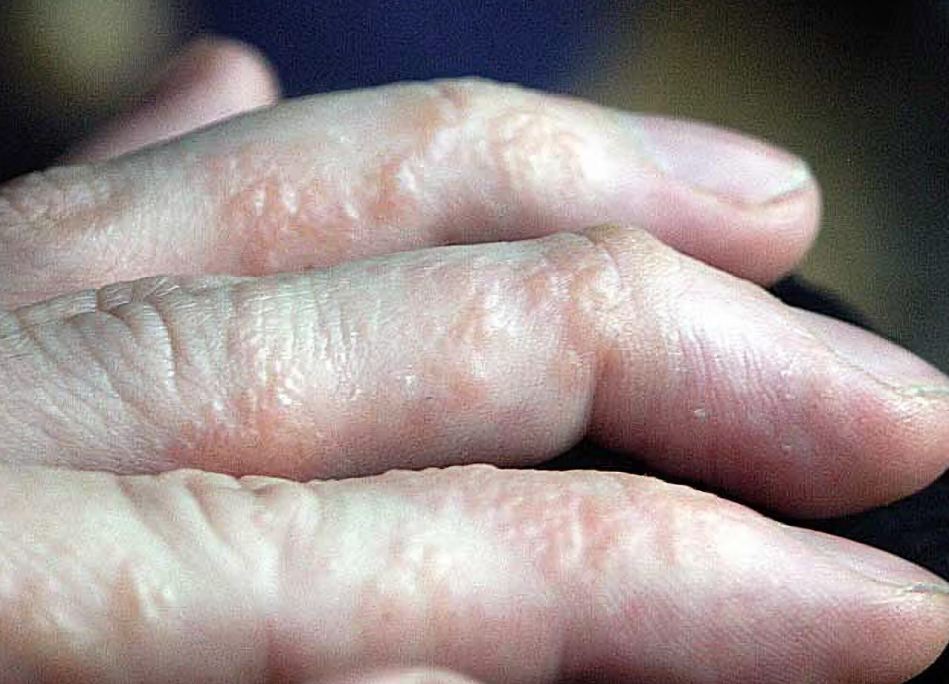
Before any blisters appear, many people experience itching, burning, or a prickly, tingling sensation where the skin will soon react. Then, clusters of tiny blisters develop — usually on palms, fingers, or soles of feet. These may be intensely itchy or painful. In some cases, the small blisters merge to form larger ones. As they heal, the skin often becomes red, cracked, dry, scaly — sometimes peeling or flaking. This can be uncomfortable and may even interfere with daily tasks like walking or using your hands normally. If the affected skin is scratched or irritated, there is also a risk of bacterial infection. Signs may include increased pain, swelling, or yellowish fluid or crust forming over the blisters.

What Causes or Triggers It
The exact cause of dyshidrotic eczema remains unknown. Experts believe it results from a mix of genetic predisposition and environmental triggers.
Certain factors appear to increase the likelihood of flare-ups:
- Allergies or sensitivities, especially to metals like nickel or cobalt (common in jewelry, coins, some clothes or hardware).
- Exposure to irritants or harsh chemicals, such as detergents, soaps, solvents, or perfumes.
- Frequent moisture or sweating on the hands or feet. Jobs or tasks that involve repeated hand-washing or wet work may worsen symptoms.
- Stress — emotional or physical stress can trigger or worsen flare-ups.
- Other skin conditions or allergies — having a history of eczema or allergic dermatitis can increase one’s vulnerability.
- Because triggers vary widely and may differ person to person, often flare-ups appear without a clear single cause.
Managing and Treating Dyshidrotic Eczema
While there is no definitive cure, many people successfully manage flare-ups and reduce their frequency with proper care and treatment.
Basic Skin Care
Use gentle, fragrance-free cleansers (avoid harsh soaps) and wash with lukewarm water rather than hot water. Moisturize often — applying unscented moisturizers several times a day helps keep skin barrier healthy and reduces dryness when the blisters heal. Avoid exposure to irritants — such as detergents, solvents, jewelry or other metal objects that may cause a reaction (consider wearing cotton-lined gloves if needed).
Medical Treatments
For more severe or persistent cases, a doctor or dermatologist may recommend:
- Topical steroid creams or ointments to ease inflammation, reduce itching and help blisters heal faster.
- Antihistamines to relieve itching, especially if symptoms disturb sleep or comfort.
- In some cases, when eczema is long-lasting or severe, stronger therapies may be considered — e.g. light therapy (phototherapy), non-steroid topical meds, or systemic treatments under medical supervision.
Lifestyle Adjustments
Because flare-ups often link to triggers and lifestyle, many people find relief by:
- Minimizing contact with known irritants or allergens (metals, harsh soaps or detergents)
- Keeping hands and feet dry and clean; changing socks/shoes regularly if sweaty
- Managing stress — a calming routine, balanced sleep or relaxation methods may help reduce flare-ups
When to Seek Medical Advice
If your blisters are very painful, leaking pus, covered in crust, or appear infected — or if the rash doesn’t improve after a few weeks — it’s important to see a doctor or dermatologist. Also see a professional if symptoms reoccur often, if daily activities (walking, using your hands) become difficult, or if skin gets thickened, cracked, or badly irritated.
Living with Dyshidrotic Eczema — What to Know
Dyshidrotic eczema can be frustrating and uncomfortable, but it’s often manageable. With good skin care, avoidance of triggers, and appropriate treatment when needed, many people lead full normal lives. Because triggers differ widely, it often takes some trial-and-error to discover what aggravates your skin — for example, a type of detergent, a ring made with nickel, constant moisture, or stress. Once triggers are identified and avoided, flare-ups tend to become less frequent or less severe. If you like, I can also expand this summary — adding common triggers and self-care routines especially for teenagers (skin-friendly habits, suggestions for everyday life, etc.). Do you want me to build that version for you now?

















